This story is part of the series Expecting worse: Giving birth on a planet in crisis, a collaboration between Grist, Vox, and The 19th that investigates how climate change impacts reproductive health — from menstruation to conception to birth.
Roger Casupang was working in a coastal clinic on the north side of Papua New Guinea, an island nation of 9 million in the southwestern Pacific Ocean, when a pregnant woman burst into his facility. She was in labor, moments away from delivering twins. She also had a severe case of malaria, a life-threatening mosquito-borne illness common in tropical countries.
Casupang, an obstetrician, quickly took stock of the situation. When the parent is healthy, a twin pregnancy is twice as risky as a single pregnancy. Meanwhile, severe malaria kills nearly half of the people who develop it during pregnancy. The woman was exhausted and delirious. Because many of his patients walked for days to get medical care for standard ailments, Casupang didn’t know which province she had come from or how long she had been traveling before she reached his clinic.
What he did know was that the woman had arrived just in time. “She was actually pushing when she came in,” he said.
Casupang, who was born in one of Papua New Guinea’s highland provinces and had been practicing medicine on the island for the better part of a decade at the time, had seen pregnant women die in less dire circumstances. Against all odds, with limited medical resources and medicines at their disposal, Casupang and the other medical professionals at the clinic were able to deliver the twins safely. Both babies weighed less than three pounds each, a consequence of their mother’s raging infection. The twins were moved to the nursery while Casupang and his fellow physicians worked to stabilize the mother. She was reunited with her babies after 10 days of intensive care. “If this case had presented in a remote facility,” Casupang said, “the narrative would have been very different.”
Casupang’s patient was lucky to survive — but she also benefited from geography. On the coast, doctors see lots of patients with malaria, and many of those patients carry antibodies that protect them from severe infection.
But malaria is on the move.

A woman sleeps with her baby in the maternity ward of a hospital in Goroka in the Eastern Highlands Province of Papua New Guinea in 2009. Jason South / Fairfax Media via Getty Images
Temperatures are rising around the world but particularly in countries where the disease is already present. That warming coaxes mosquitoes toward higher elevations, even as temperatures have historically been too cold for the insects to thrive. In these high-altitude areas, mosquitoes are feeding on people who have never had malaria before — and who are much more susceptible to deadly infections.
“When malaria hits new populations that are naive, you tend to get these explosive epidemics that are severe because people don’t have any existing immunity,” said Sadie Ryan, an associate professor of medical geography at the University of Florida.
Pregnant people living in highland regions who have never had malaria before are worst-positioned to survive the bite of an infected mosquito. The very act of becoming pregnant creates a potentially deadly vulnerability to malaria. The placenta, the new organ that forms to nourish the fetus, presents new receptors for the disease to bind to.
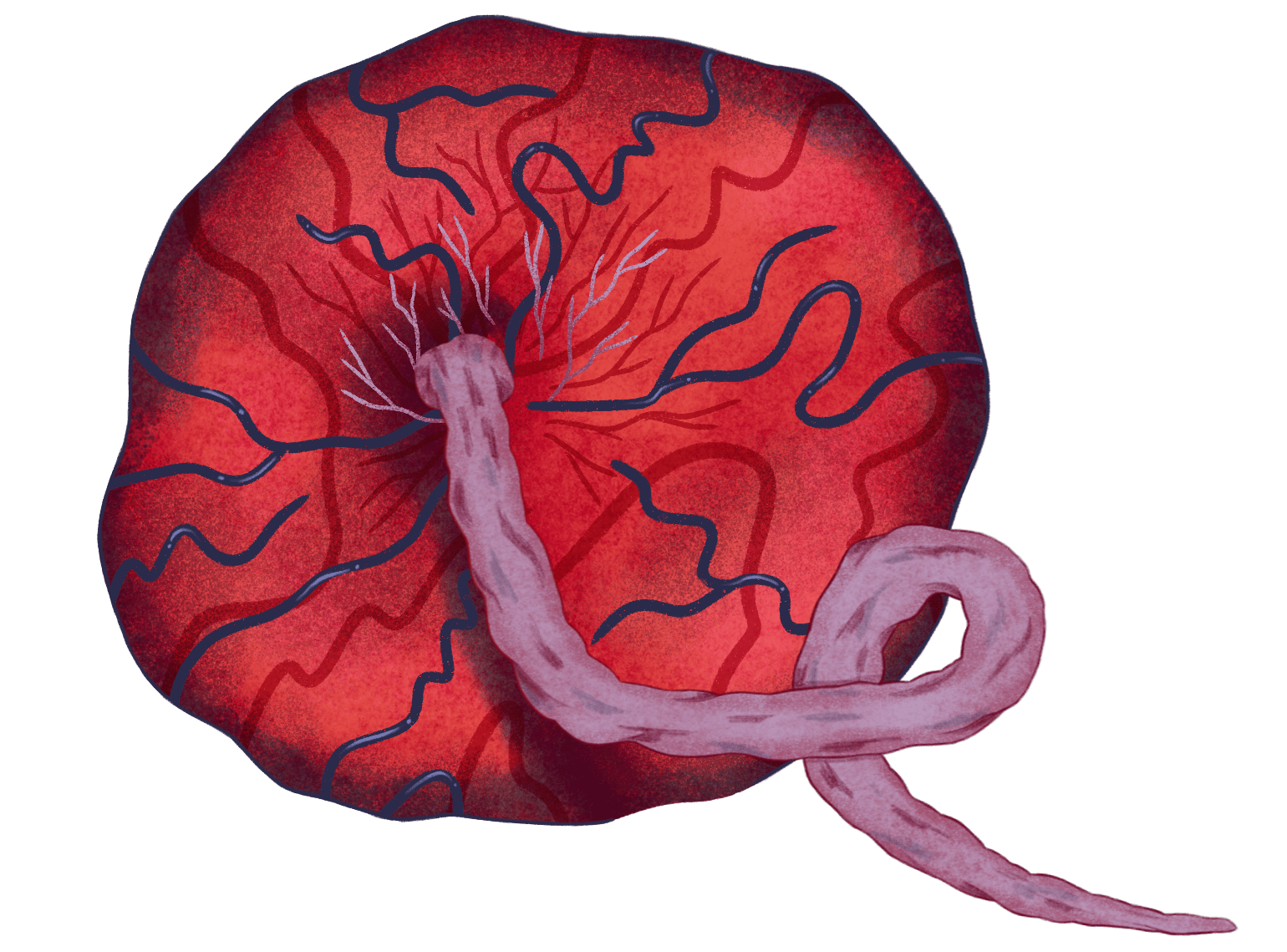
Amelia K. Bates / Grist
Pregnant women are three times more likely to develop severe malaria compared to nonpregnant women. For people who can become pregnant, the climate-driven upward movement of malaria mosquitoes poses nothing less than an existential threat.
“In Western countries, especially where malaria is not endemic, there is this perception that malaria has been around for so long that we already know how to deal with it,” said Deekshita Ramanarayanan, who works on maternal health at the nonpartisan research organization the Wilson Center.
But that was never the case, and the perception is especially flawed now, as climate change threatens to rewrite the malaria-control playbook. “Pregnant people are hit with this double risk factor of climate change and the risks of contracting malaria during pregnancy,” Ramanarayanan said.

Hundreds of millions of people get malaria every year, and an estimated 2.7 million die from it, mostly in tropical and subtropical regions. In 2022, 94 percent of global malaria cases occurred in sub-Saharan Africa. High rates of the disease are also found in Central America and the Caribbean, South America, Southeast Asia, and the western Pacific. Papua New Guinea registered over 400,000 new cases in 2022. That same year the country accounted for 90 percent of the malaria cases in the western Pacific.
Malaria is carried by dozens of species of Anopheles mosquitoes, also known as marsh or nail mosquitoes. Anopheles mosquitoes carry a parasite called Plasmodium — the single-cell genus that causes malaria in birds, reptiles, and mammals like humans.
When the bite of an Anopheles mosquito introduces Plasmodium into the human bloodstream, the parasites travel to the liver, where they lurk undetectably and mature for a period ranging from weeks to a year. Once the parasites reach maturity, they venture out into the bloodstream and infect red blood cells. The host often experiences symptoms at this stage of the infection — fever, chills, nausea, and general, flu-like discomfort.
The earlier a malaria infection is caught, the better the chances that antimalarial medications can help prevent the development of severe malaria, when the disease spreads to critical organs in the body.
Pregnancy primes the body for infection.
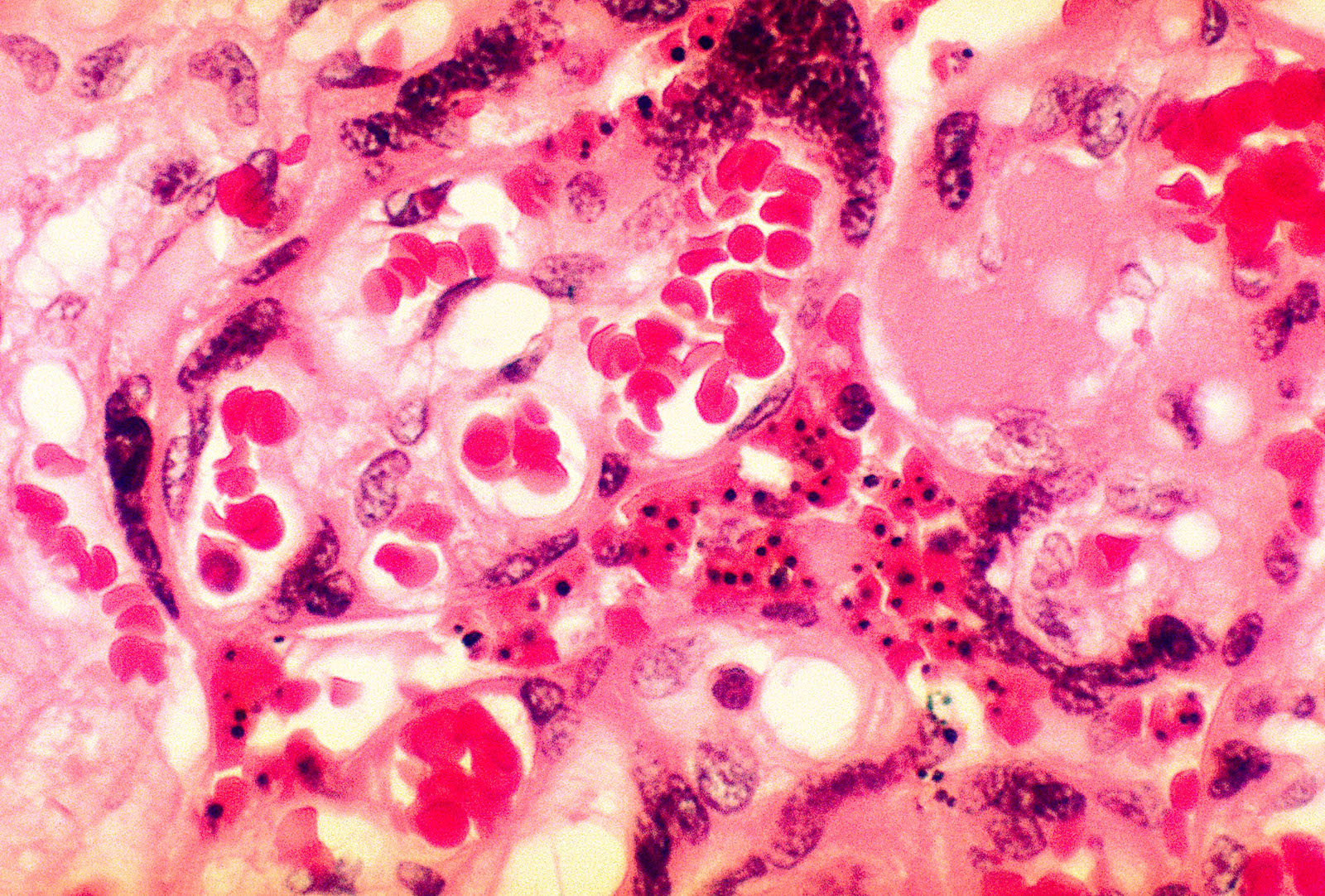
A photomicrograph of placental tissue revealing the presence of the malarial parasite Plasmodium falciparum. BSIP / UIG Via Getty Images
The immune system, when it is functioning properly, engages an arsenal of weapons to ward off bacteria, viruses, and other pathogens. But pregnancy acts like an immunosuppressant, telling the defense system to stand down in order to ensure the body does not inadvertently reject the growing baby. “Your immune system is, on purpose, dialed back so that you can tolerate the fact that you have this fetus inside of you,” said Marya Zlatnik, an obstetrician and gynecologist at University of California, San Francisco Medical Center.
Then there’s the added strain of supplying the baby with enough nutrients, vitamins, and minerals. The body must work overtime to provide for the metabolic needs of two. This factor, exacerbated by poverty, malnutrition, and subpar medical infrastructure in countries where malaria is commonly found, poses enormous challenges to maternal and fetal health. A malaria infection on top of those existing vulnerabilities introduces another, even more challenging set of obstacles.

The disease can produce severe maternal anemia, iron deficiency, or it can spread to the kidneys and the lungs and cause a condition known as blackwater fever. The disorder makes patients jaundiced, feverish, and dangerously low on vitamins crucial for a healthy pregnancy.
“It’s pretty much synonymous with death for many patients up in the rural areas,” Casupang said. Research shows that malaria may be a factor in a quarter of all maternal deaths in the countries where the disease is endemic.
A woman with her newborn baby in the birthing suite at a hospital in Goroka in 2009. Jason South / Fairfax Media via Getty Images
Plasmodium parasites have spikes on them, similar to the now-infamous coronavirus spike proteins, that make them sticky and prone to clogging up organs. If Plasmodium travel to the placenta, the parasites bind to placental receptors and cause portions of the placenta to die off. “It changes the architecture of the placenta and the ways nutrients and oxygen are exchanged with the fetus,” said Courtney Murdock, an associate professor at Cornell University’s department of entomology. The placental clots interfere with fetal growth, and they’re one of the reasons why a pregnant woman is between three and four times more likely to miscarry if she has a malaria infection, and why babies born to mothers sick with malaria come out of the womb malnourished and underweight.
“You see the placenta start to fail,” Casupang said. Fetal mortality is closely tied to how much of the placenta becomes oxygen deprived. “The babies come out with very low birth weights,” he said. If the placental clots are extensive, “they usually die.”
In 2020, approximately 122 million pregnancies — about half of all pregnancies worldwide that year — occurred in areas where people were at risk of contracting malaria. A 2023 study estimated that 16 million of these pregnancies ended in miscarriage, and 1.4 million in stillbirth.
Researchers don’t know exactly how many of those miscarriages and stillbirths occurred in individuals who were bitten by malaria-infected mosquitoes.
However, the World Health Organization estimates that approximately 35 percent of pregnant people in African countries with moderate to high malaria transmission were exposed to the disease during pregnancy in 2022. A widespread lack of health data in poor countries makes it nearly impossible to know how many of those infections resulted in maternal, fetal, or infant death. “Unfortunately, it is only safe to say that we do not have good morbidity estimates at this point,” said Feiko ter Kuile, chair in tropical epidemiology at the Liverpool School of Tropical Medicine.
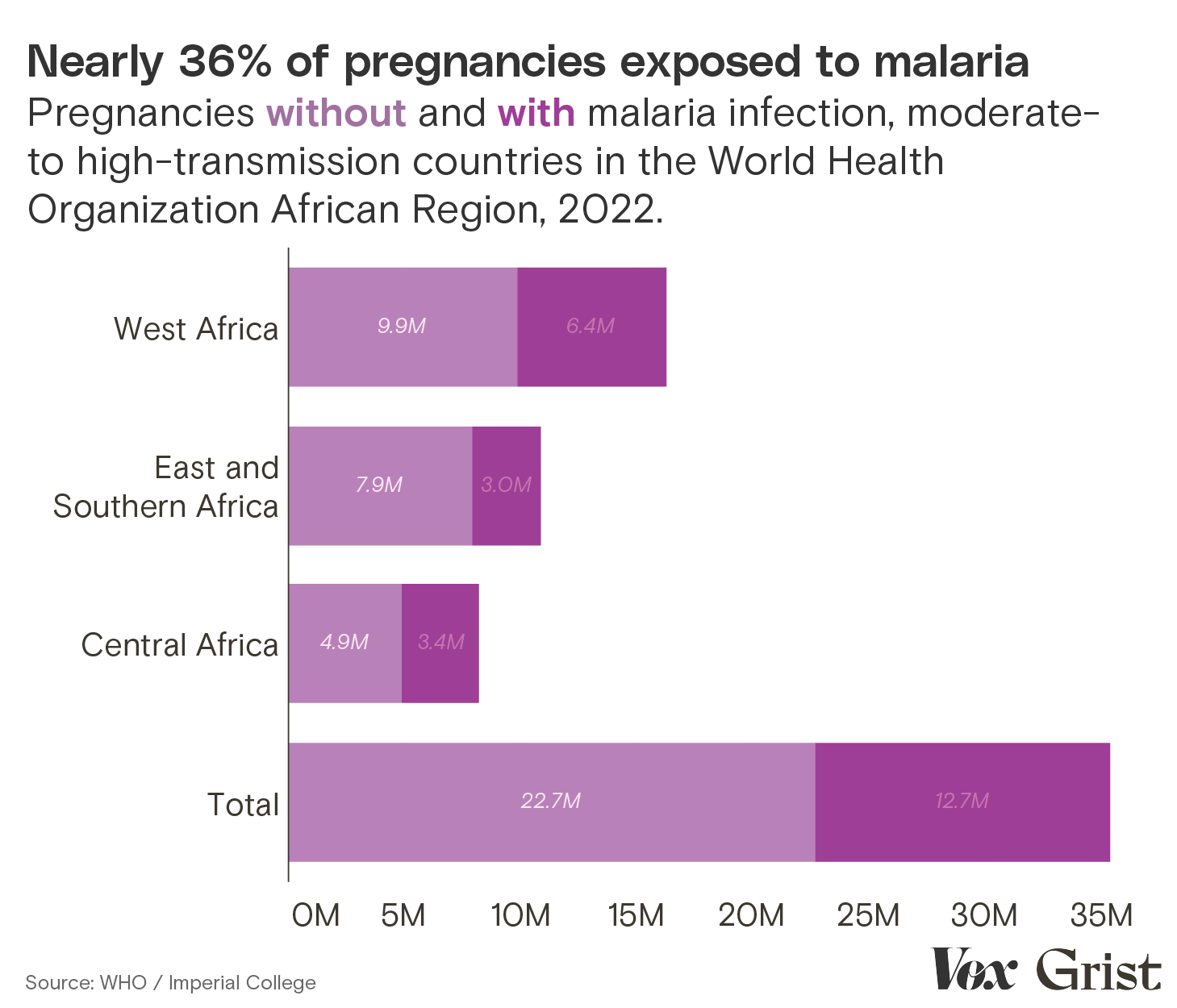
Clayton Aldern / Grist
Researchers have said that out of all the high-impact infectious diseases — including Ebola, mpox (formerly known as monkeypox), and MERS — malaria is the “most sensitive to the relationship of human populations to their environment.” In Papua New Guinea, the coastal zones that sit near or at sea level have long had environmental conditions that foster the development and spread of the Anopheles mosquito. Cases of malaria topped 1.5 million in 2020, and the vast majority occurred in the nation’s lowlands.
At 4,000 feet or more above sea level, where some 40 percent of the Papua New Guinean population lives, temperatures have historically been too cold for Anopheles mosquitoes to thrive year-round. There have been seasonal outbreaks of malaria in those zones, but the background hum of malaria present in the lowlands largely disappears above the 4,000 feet mark. At 5,200 feet above sea level, periodic freezes kill mosquitoes and prevent them from establishing widely, making malaria infections there very rare.
But climate change is expanding the areas where Anopheles mosquitoes and the Plasmodium they carry flourish by fostering warmer, wetter environments. Mosquitoes thrive in the aftermath of big storms, when the insects have ample opportunity to breed in standing pools of water.
At the same time, higher-than-average temperatures almost everywhere in the world mark the beginning of a new chapter in humanity’s long struggle to contain mosquitoes and the diseases they carry. Anopheles mosquitoes grow into adults more quickly in warmer weather, and longer warm seasons allow them to breed faster and stay active longer.
This poses problems in areas where Anopheles mosquitoes are already prevalent, and in regions the insects are poised to infiltrate. The mountainous regions of the world — the Himalayas, the Andes, the East African highlands — are thawing as average global temperatures climb. What used to be an inhospitable habitat is becoming fertile ground for malaria transmission.

Women pick strawberries in a highland field in Enga Province, Papua New Guinea, in December 2019.
Betsy Joles / Getty Images

Piglets stand on the road near Kapandas village in the highlands of Papua New Guinea in December 2019.
Betsy Joles / Getty Images
Like their mosquito hosts, Plasmodium parasites are sensitive to temperature. The two most common strains, Plasmodium falciparum and Plasmodium vivax, like temperatures in the range of 56 to 95 degrees Fahrenheit. The warmer the weather, the more quickly the parasites are able to reach their infectious stage. A study that examined temperatures suitable to Plasmodium in the western Himalaya mountains predicted that, by 2040, the mountain range’s high-elevation sites — 8,500 feet above sea level — “will have a temperature range conducive for malaria transmission.”
There’s little data on the rate at which Anopheles mosquitoes and the parasites they carry are moving upward in Papua New Guinea, but research shows temperatures across Papua New Guinea were, on average, just under 1 degree Celsius (1.8 degrees F) warmer between 2000 and 2017 than they were a century prior. A report conducted by the World Bank Group noted that this temperature rise “has been fastest in the minimum temperatures,” meaning climate change jeopardizes the overnight low temperatures that are so essential to mosquito control. Anecdotally, doctors and nurses working in the country’s colder regions say they have seen a familiar pattern begin to change.
Stella Silihtau works in the emergency department at the Eastern Highlands Provincial Health Authority in Goroka, a town of 20,000 that sits at 5,200 feet above sea level on a major road that connects the scattered highland cities and towns to the communities along the coast. Silihtau and her colleagues are no strangers to malaria. Hundreds of people in Goroka and surrounding highland towns grow cash crops like coffee, tea, rubber, and sugarcane and ferry them down to the coast every week to sell to plantations and community boards. The highland dwellers are bitten by mosquitoes at lower elevations, and end up at the hospital where Silihtau works weeks later, sick with malaria. Over the past year, she’s seen unusual cases starting to crop up.
“We’ve been seeing a lot of patients that are coming in with malaria,” said Silihtau, who grew up in the lowlands. Many of these cases have been in people who have not traveled at all. “We’ve seen mild cases, severe cases, they go into psychosis,” she said.

A fire set to repel mosquitoes in Milne Bay Province, Papua New Guinea. Eric Lafforgue / Art in All of Us / Corbis via Getty Images
Silihtau and her colleagues don’t have the time or staff to keep close track of how many locally acquired malaria cases have been treated at the hospital over the past year. But Silihtau estimates that when she first started working at the hospital in Goroka two years ago, she saw one case per eight-hour shift, or none at all. Now, she sees between two and three cases of malaria per shift, some of them in individuals who have not traveled outside the boundaries of Papua New Guinea’s highland zones. “It’s a new trend,” Silihtau said.

The new dangers that the upward movement of malaria mosquitoes pose to pregnant people are obfuscated by positive signals in malaria cases globally.
Global malaria deaths plummeted 36 percent between 2010 and 2020, the dive driven by wider implementation of the standard, relatively low-cost treatments that research shows are incredibly effective at preventing severe infections: insecticide-treated mosquito nets, antimalarial drugs, and malaria tests.
This promising trend stalled in 2022, when there were an estimated 249 million cases of malaria globally — up 5 million from 2021. Much of the increase can be attributed to the COVID-19 pandemic, which slowed various global infectious disease control efforts as health care systems tried to contain an entirely new threat. Funding for malaria control is also falling short. Countries spent a total of $4.1 billion on malaria in 2022, nowhere near the $7.8 billion in funding the World Health Organization says is necessary annually to reduce the global health burden of the disease 90 percent by 2030.
Meanwhile, cases have been rising in step with the spread of a mosquito called Anopheles stephensi, a species that can carry two different strains of Plasmodium and, unlike the rest of its Anopheles brethren, thrives in urban environments. Efforts to control malaria in both urban and rural settings are stymied by the quickening pace and severity of extreme weather events, which scramble vaccination and mosquito net distribution campaigns, shutter health clinics, and interrupt medical supply chains. Record-breaking storms, which destroy homes and public infrastructure and create thousands of internal migrants, force governments in developing countries to choose where to allocate limited funding. Infectious disease control programs are often the first to go.
The world’s slowly warming highland regions are one small thread in the web of factors influencing the prevalence of malaria. But because of the lack of immunity among populations in upper elevations, the movement of malaria into these zones poses a unique threat to pregnant people — one that may grow to constitute a disproportionate fraction of the overall impact of malaria as climate change continues to worsen.
“Pregnant women are going to be a high-risk population in highland areas,” said Chandy C. John, a professor and researcher at Indiana University School of Medicine who has conducted malaria research in Kenya and Uganda for 20 years. John and his colleagues are in the process of analyzing their two decades of health data to try to tease out the potential effects of climate on malaria cases. “What are we seeing in terms of rainfall and temperature and how they relate to risk of malaria over time in these areas?” he asked. His study will add to the small but growing body of research on how temperature shifts in high elevations contribute to the prevalence of malaria.

Controlling and even eradicating malaria isn’t just possible; it has already been done. Dozens of countries have banished the disease; Cabo Verde recently became the third African country to be certified as malaria-free. “Malaria is such a complex disease,” said Jennifer Gardy, deputy director for malaria surveillance, data, and epidemiology at the Bill and Melinda Gates Foundation, “but that complexity is kind of beautiful because it means we’ve got so many different intervention points.”
In addition to the typical interventions such as mosquito nets, the Papua New Guinea National Department of Health has had some success with medical therapies for people who develop malaria infections while pregnant. Doctors there and in many other malaria-endemic places use intermittent preventive treatment on pregnant women. The antimalarial is administered orally as soon as patients learn they are pregnant and, if taken on regularly, can significantly reduce the chances of severe malaria over the course of gestation. The treatment remains difficult to access in highland regions, as malaria has historically been uncommon there. If governments and hospitals pay attention and get these medicines into places where rising temperatures are changing climatic constraints on mosquitoes, they will save lives.

A mother feeds her newborn baby in the maternity ward of a hospital in Goroka in 2009. Jason South / Fairfax Media via Getty Images
The smartest solutions are those that address malaria as a symptom of a wider system of inequity. Papua New Guinea is a “patriarchal society where men get the best treatment,” Casupang, who now works for an international emergency medicine and security company called International SOS, said. “Women are pretty much regarded as commodities.” Most married women must seek permission from their husbands to seek medical care at a facility, and permission is not always granted. Many women are also prevented from seeking medical attention by poverty, by the quality of the roads that connect rural villages to cities, and because they don’t recognize the symptoms of malaria or understand the risks the infection poses to themselves and their unborn children, Casupang said. Just 55 percent of women in Papua New Guinea give birth in a health facility, a partial function of the fact that the country currently has less than a quarter of the medical personnel it needs to care for mothers, babies, and children.
“There are quite a number of factors that will determine the outcome of a mother that has malaria,” Casupang said. “The most important thing is access to a health care facility.” He’s one of many experts who argue that better infrastructure, improvements in education, and the implementation of policies that protect women and girls double as malaria control measures — not just in Papua New Guinea but everywhere poverty creates footholds for infectious diseases to take root and flourish.
“Education, a living wage, sanitation, and all of these other very basic things can do so much for a disease like malaria,” John said. “It’s not a mosquito net or a vaccine, but it can make such a huge difference for the population.”
>>> Read full article>>>
Copyright for syndicated content belongs to the linked Source : Grist – https://grist.org/health/fertility-climate-change-pregnancy-malaria-placenta-mosquito/










