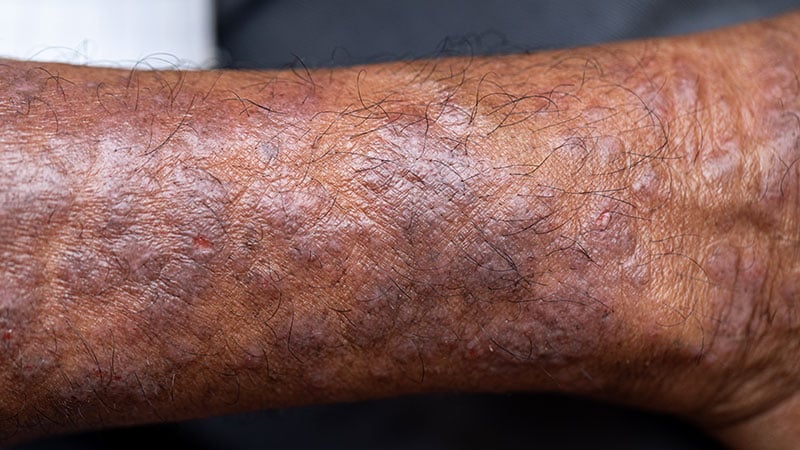
SAN DIEGO — Among patients with skin of color and moderate to severe atopic dermatitis (AD) who underwent 16 weeks of treatment with lebrikizumab, 68% achieved a 75% reduction in the Eczema Area and Severity Index (EASI-75), interim results from a novel phase 3b trial showed.
Lebrikizumab, a novel monoclonal antibody being developed by Eli Lilly and Co, binds with high affinity to interleukin (IL)–13, thereby blocking the downstream effects of IL-13 with high potency, one of the study investigators, Jill S. Waibel, MD, a dermatologist in Miami, Florida, said at the annual meeting of the American Academy of Dermatology. Though the efficacy and safety of lebrikizumab to treat moderate to severe AD have been established in phase 3 studies, including subset analyses by race and ethnicity, “there is a paucity of data to guide the treatment of moderate-to-severe AD in populations traditionally under-represented in clinical trials, including patients with skin of color,” she said.
During a late-breaking abstract session, Waibel presented interim 16-week results from ADmirable, a phase 3b, open-label, 24-week study, was the first study to evaluate the safety and efficacy of lebrikizumab in adult and adolescents with skin of color and moderate to severe AD. At baseline and at 2 weeks, patients received a 500-mg loading dose of lebrikizumab. Through week 16, they received a 250-mg dose every 2 weeks. The study’s primary endpoint was the proportion of patients who achieved a 75% reduction in EASI-75 at week 16. “If they achieved the primary endpoint at week 16, they went to a 250-mg dose every 4 weeks,” Waibel said. “If they did not achieve that [primary endpoint] they stayed on the 250-mg dose every 2 weeks.”
The analysis included 50 patients with skin types IV, V, and VI who self-reported their race as Black or African American, American Indian or Alaska Native, Asian, and Native Hawaiian or Other Pacific Islander. They had chronic AD for at least 1 year, moderate to severe disease at baseline, a history of an inadequate response to topical medications, and were naive to biologics indicated for the treatment of AD.
Week 16 outcomes of interest were the EASI, the Investigator’s Global Assessment (IGA) of 0 or 1, the Pruritus Numerical Rating Scale (NRS), and PDCA-Derm, a scale developed by Eli Lilly and Co that was used to compare postinflammatory lesions to unaffected adjacent normal skin. All data for statistical analyses were summarized as observed.
At baseline, the mean age of the 50 patients was 42 years, 46% were women, their mean body mass index was 30.2, and the mean age at AD onset was 23 years. Most study participants (80%) were Black or African American, 14% were Asian, and 6% were American Indian or Alaska Native; 78% were not Hispanic or Latino and 22% were Hispanic or Latino. The mean EASI score was 28.1, the mean body surface area affected was 41.7%, and the mean Pruritus NRS score was 7.2 out of 11. According to the PDCA-Derm scale, 18% of patients had hypopigmented lesions, and 54% had hyperpigmented lesions.
After 16 weeks of treatment, 68% of patients achieved an EASI-75 response, whereas 46% achieved an EASI-90 response, Waibel reported at the meeting. In addition, 39% of patients achieved an IGA score of 0 or 1, 56% achieved a ≥ 4-point improvement on the Pruritus NRS, and 66% achieved a ≥ 3-point improvement on the Pruritus NRS. The PDCA-Derm score identified improvement in postinflammatory hyperpigmented lesions in 12 of 21 patients and improvement to normal skin tone in six of 21 patients.
“I have a large population [with skin of color in my practice],” Waibel said. “I usually tell my [patients with postinflammatory hyperpigmentation] that it takes 6 months to see improvement. In this study, we saw patients achieve improvement in skin tone in a 4-month timeframe. PIH is sometimes more distressing than a primary condition, whether it’s acne or atopic dermatitis. In this case, it was surprisingly improved with lebrikizumab.”
No new safety signals or serious adverse events were observed. “This is very exciting because it’s the first time there has been a trial focusing on [patients with skin of color] with moderate to severe eczema in skin types IV-VI,” Waibel said.
In an interview, the study’s lead investigator, Andrew Alexis, MD, MPH, vice chair for Diversity and Inclusion in the Department of Dermatology and professor of clinical dermatology at Weill Cornell Medicine, New York City, said that the interim results from this study ” add valuable, clinically relevant data on the treatment of moderate to severe AD in patient populations with skin of color.”
“An interesting finding,” he continued, “was that improvement in postinflammatory hyperpigmented lesions was seen in 12 of 21 patients and improvement to normal skin tone was observed in six of 21 patients at week 16. This is particularly relevant to patients with skin of color who frequently suffer from pigmentary changes in association with their AD.”
Lebrikizumab was approved in November 2023 in Europe for the treatment of moderate to severe AD in people aged 12 years or older and is currently under review by the US Food and Drug Administration for treatment of AD.
Both Waibel and Alexis disclosed numerous conflicts of interest from various pharmaceutical companies, including serving as a consultant and/or advisor to Eli Lilly and Co.
>>> Read full article>>>
Copyright for syndicated content belongs to the linked Source : Medscape – https://www.medscape.com/viewarticle/lebrikizumab-found-effective-patients-eczema-darker-skin-2024a10004om